Living with the Reality of Dementia
Japan’s Failing Nursing Care Insurance System
Society- English
- 日本語
- 简体字
- 繁體字
- Français
- Español
- العربية
- Русский
The Helper Shortages Threatening Elderly Health
People with family members requiring care due to dementia and other conditions often struggle ceaselessly to cope with the condition of their loved one. Their main support is provided by specialized nursing care services. Japan’s nursing care insurance system, paid for with premiums levied from the age of 40, provides 70%–90% coverage for in-home nursing, attendance at day care facilities, and short-term and permanent nursing home placement.
But there are disparities between the service provided in urban versus rural areas, despite insurance premiums being equal.
Around 80% of Nagano Prefecture is mountainous, with urban centers located in scattered basins. Nursing care providers struggle to serve residents in the mountainous areas. Nozomi is an aged care facility operating in renovated old buildings on a hill in the suburbs of the prefectural capital of Nagano. It principally offers a day care service, collecting patients from their homes, feeding and bathing them, and providing functional training and nature walks before returning them home.

The Nagano cityscape viewed from the Nozomi aged care facility. (© Mochida Jōji)
But Nozomi is unable to offer in-home nursing care due to a lack of staff.
In comparison with other fields, the labor shortage in the nursing industry is particularly grave. Nozomi’s head, Denda Kagemitsu, struggles with the issue, explaining that his organization is aware of the importance of in-home care, but lacks the staff to provide such services. “In-home care requires traveling half an hour or more into the mountains, visiting one home at a time. It’s much more efficient for us to bring multiple people to one location. It also greatly reduces fuel costs.”
He also points out that providers of in-home care in some mountainous areas only manage to see patients once a week.

Nozomi’s vehicle fleet is essential to transport patients to and from the facility. (© Mochida Jōji)
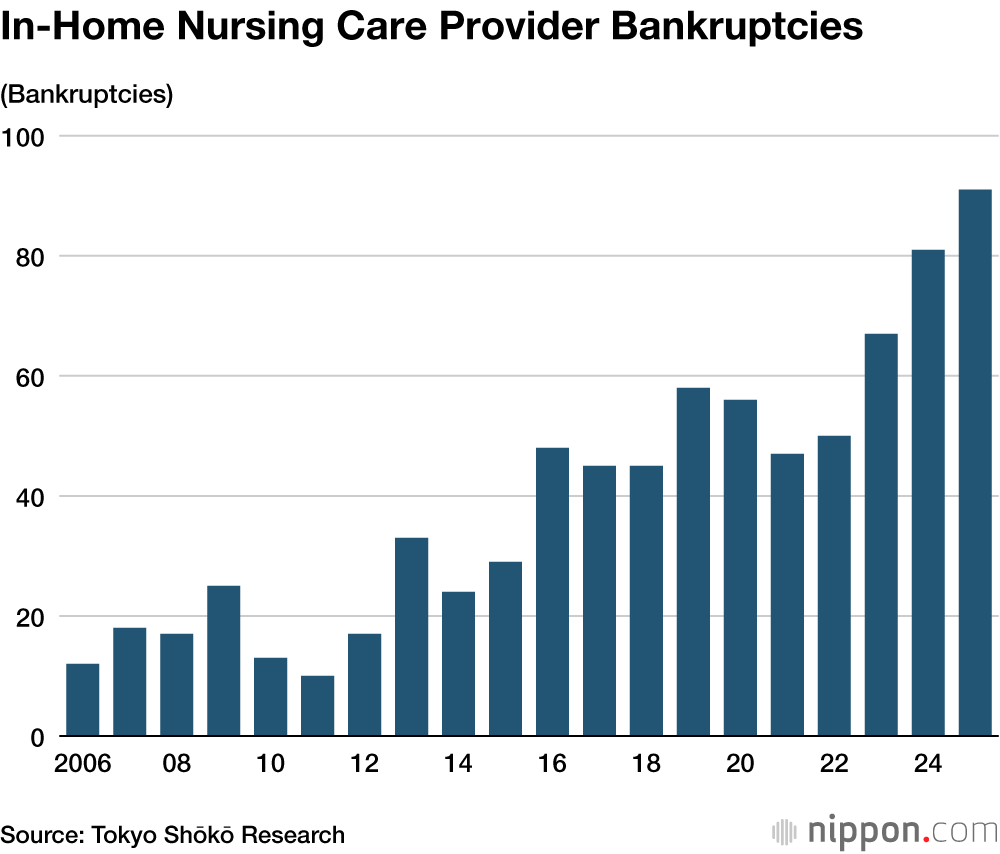
Across Japan, in-home nursing care providers in particular face financial difficulties. Revisions made in fiscal 2024 lowered nursing compensation rates, causing greater staff shortages. In 2025, this led to the bankruptcy of 91 providers, a record high for the third consecutive year, according to Tokyo Shōkō Research.
Wage Disparity
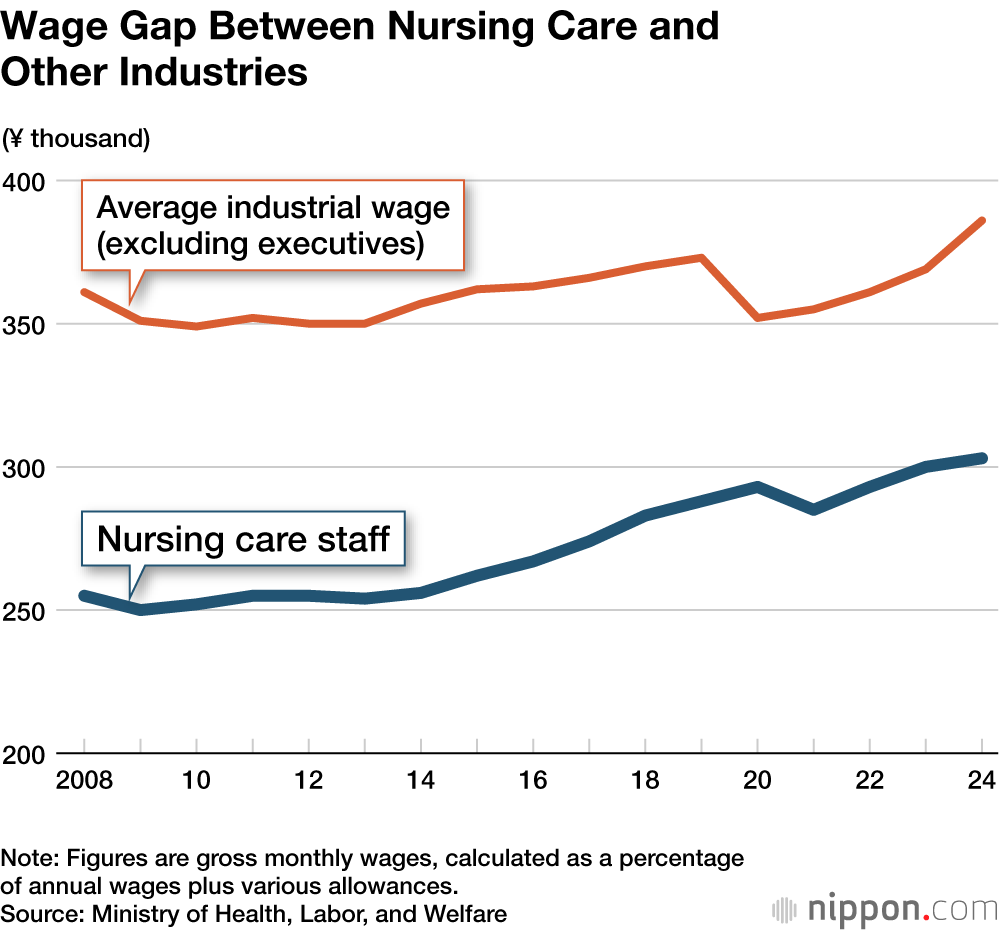
Providers of in-home and other nursing care struggle due to the low wage allowance paid by nursing care insurance, which has led to chronic staff shortages. Meanwhile, Japan’s declining population is producing fierce competition among a range of industries to secure workers. According to a survey conducted by the Ministry of Health, Labor, and Welfare, the average wage in nursing care was ¥303,000/month, which is ¥83,000 lower than the average across all industries.
Denda strives to attract staff through word of mouth, but is constantly challenged by the task of rostering his 22 staff members, 14 of whom are part-timers. Many of these workers have yet to obtain certification as care workers, meaning that they earn a lower wage according to the official pay schedule. Moreover, the average age of staff is 57 and rising—in winter, he is sometimes unwilling to send them out to drive on the icy roads.
He has begun looking to the foreign labor pool to ensure survival of the business, employing a worker from Myanmar in 2024. This year, he hopes to employ one more, but securing foreign workers is not easy. “Many foreigners intend to send money back home, so they focus on the potential earnings. The weak yen reduces the value of their remittances, so many are now seeking work in Australia or South Korea, and Japan is not even on their radar.”

Denda says he hopes to employ more foreign staff. (© Mochida Jōji)
Rising commodity prices also place pressure on business. Nursing care insurance pays a fixed remuneration to providers based on their headcount, not their actual costs; price increases result in reduced profits. Although the cost of fuel for their vehicles and for winter heating is relatively stable as of the writing of this article in January 2026, it remains high. Furthermore, there have been steep hikes in the price of tires, not to mention the rice needed for patients’ meals.
Major nursing care operators are quick to withdraw from less profitable areas. In recent years, two companies pulled out of the city of Nagano. Denda stresses, though: “Companies like ours have a responsibility to the community. We can’t simply tell patients we’ll end services in a week.”
No Longer Just a Rural Issue

According to Yūki Yasuhiro, nursing care in Japan risks becoming a “system without services.” (© Mochida Jōji)
By 2035, Japan’s postwar baby-boomers will be aged 85 and over, which will cause a steep rise in needs for dementia and other nursing care. This raises concerns as to whether nursing care services will keep pace.
Funds to secure staff and to ensure business stability are contributed by the nursing care insurance system, funded by taxes, insurance premiums, and patient copayments. According to Professor Yūki Yasuhiro of the Shukutoku University School of Social Welfare, unless radical changes are made to funding, there is a risk of it becoming a “system without services.” He warns: “Signs of this are already emerging, and it is no longer an issue impacting rural areas alone.”
He notes in particular: “Unless the wages of nursing care staff are increased by at least ¥50,000 or ¥60,000 a month, it will become impossible to find workers.” He calculates that this will require an additional ¥1.4 trillion in funding annually.
Contributions and Benefits
What options are available for reforming Japan’s nursing care insurance system?
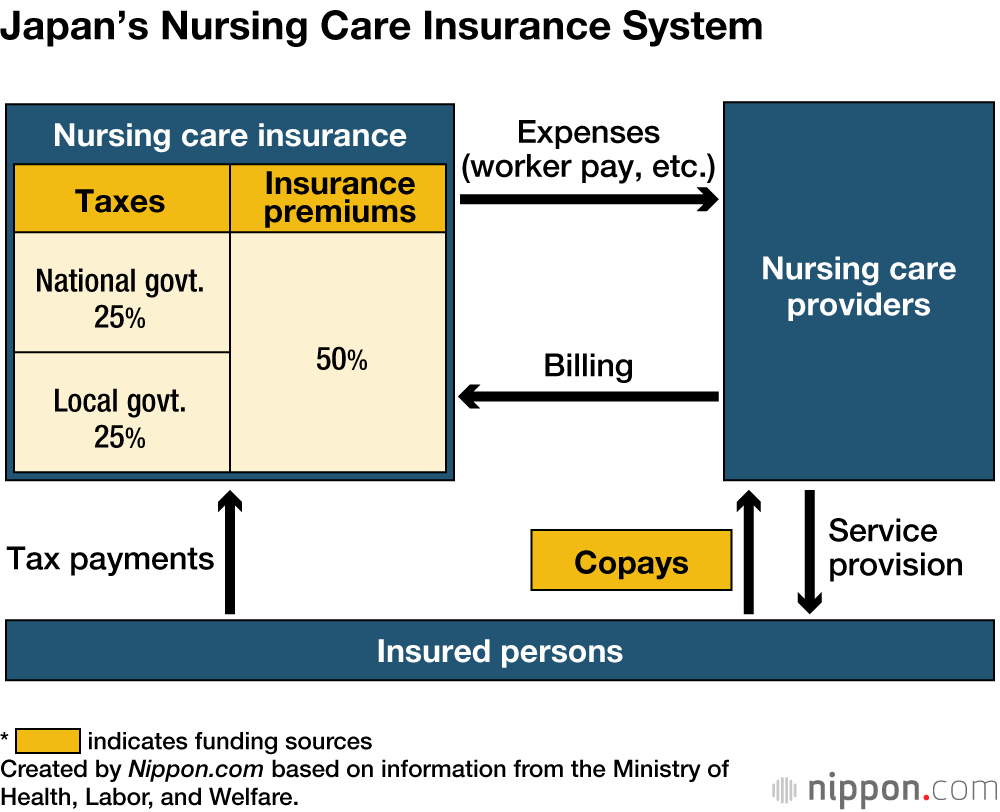
Currently, national and local governments each provide 25% of funding for the system, with the remaining 50% coming from insurance premiums, levied on all people aged 40 and above. Users of care services make copayments of either 10%, 20%, or 30% according to their income level.
As the number of elderly people requiring nursing care continues to rise, the total cost of nursing care insurance had grown to nearly ¥12 trillion as of 2022. Consequently, insurance premiums are also being increased. When the system was launched in fiscal 2000, the average national premium was ¥2,911 per person per month, but over time this has more than doubled, now averaging ¥6,225. While the majority of patients make 10% copayments, deliberation is currently underway to increase the proportion of patients paying 20% from fiscal 2027 onward.
Yūki points out that for elderly patients, whose annual income has typically plateaued, “As they struggle with rising living costs, increases to the insurance premiums and copayments will lead to some people shunning care.”
In addressing social welfare, including nursing care insurance, Prime Minister Takaichi Sanae announced a policy to establish a nonpartisan national council, stating the need for “national debate aimed at revising contributions and benefits.” The fiscal 2025 supplementary budget allocated increased funding for nursing care facilities and employee remuneration. In contrast, a key policy of Nippon Ishin no Kai, junior coalition partner to the ruling Liberal Democratic Party, is to increase take-home income for white-collar workers by reducing social welfare insurance premiums.
But although the burden of insurance premiums on the working age population is high, reducing this would inevitably cause a decline in the service provided. According to Yūki, “Subsidies and small remuneration increases are not enough. Without a permanent funding source and significant boost to pay levels for care workers, we will be unable to maintain the system.”
The only solution he sees is increasing taxes. One suggestion is to tax the financial assets of the affluent to avoid intergenerational wealth gaps. Another is to increase corporate taxes. Companies are seeing an increase in staff being forced to retire to care for their parents. Raising corporate taxes can benefit companies faced with staffing difficulties by helping to reverse this trend.
Yūki is concerned that “unless we act now, in ten years’ time, there will be a class of people unable to access nursing care.”
(Originally published in Japanese. Banner photo: Patients and staff of the Nozomi aged care facility admire the cherry blossoms in Nagano, Nagano Prefecture. © Denda Kagemitsu.)